Like many other Americans, the first thing Steve White does after he wakes up in the morning is step on a scale.
But though it looks like the old weigh-yourself-for-a-nickel devices that used to be in penny arcades, the contraption on his living room floor does a lot more than measure his weight.
It's actually a remote patient-monitoring device for people with congestive heart failure.
The 51-year-old White was diagnosed in early January with cardiomyopathy — that’s weakening of the heart muscle.
“I thought it was the flu," White recalled, "because I couldn’t breathe well, especially when I was laying down and I was coughing a lot and couldn’t get a deep breath.”
White now takes a variety of medications every day. He’s had to stop drinking and adopt a low-sodium diet.
“I had to change my life," White said. "And I lost 50 pounds because of it.”
To make sure his weight and other risk factors stay under control, White uses this special scale, called Cardiocom.
People like White who suffer from severe chronic illnesses like heart disease can easily rack up enormous medical costs.
If their conditions aren’t controlled properly, they’re forced to make frequent trips to the hospital.
Remote sensors and other telemedicine devices can be a game-changer.
Because White’s heart doesn’t pump well, his body tries to make up for it by retaining fluid in his lungs. This can be dangerous.
The Cadiocom scale can detect as little as one-tenth of a pound of excess fluid.
“Two times in the last couple of months, I’ve gained and lost five pounds in one day," White recalled. "Pure fluid in my body, and that scale tells me that.”
The scale also electronically transmits the information to Odette Crandall in her downtown San Diego office.
She’s a congestive heart failure case manager at Sharp Rees-Stealy Medical Centers.
As soon as White finishes weighing himself, the data appear on Crandall's computer monitor.
“I get all the transmissions from Steve every day," Crandall explained. "If Steve signaled an alert, and depending on the questions that he answers, if he’s having problems, issues with the weight, breathing, or swelling, then he will show up on my acute list.”
When someone shows up on her acute list, Crandall checks the patient’s answers to the Cardiocom questions from that morning.
“The ones that you see in red," she said, pointing at her computer screen, "those are acute symptoms, and those are the ones that are going to bring him to the acute list if he answers positive.”
Crandall can also review patient data from the last 30 days.
Then she’ll call the patient to find out what’s up:
“Hi, good morning. This is Odette Crandall. I’m calling from the Sharp Rees-Stealy heart failure program in Cardiocom. Can I speak to Steven White?”
Crandall said sometimes patients’ issues on a particular day are not associated with their heart conditions.
“If it’s related to the heart failure, and there’s concerns, then I communicate with the doctor(s), and let them know what’s going on," she said.
Crandall is one of three case managers at Sharp Rees-Stealy who keep tabs on heart patients. Each manager handles about 130 patients.
Sharp’s population health department also tracks people with asthma.
Janet Appel directs the department.
She explained telemedicine devices like Cardiocom enable patients with severe chronic diseases to manage their conditions at home. Case managers can use their daily health updates to make sure patients are staying on track.
“And actually be able to provide some interventions via medication or instruction," Appel said, "to keep the patient from going to the emergency room or even being admitted to the hospital."
Appel pointed out some patients don’t feel comfortable calling their doctor about every little problem. What’s more, doctors aren’t that easy to reach, but her case managers are.
"And this way," Appel said, "they have someone who’s here, who answers the phone, who can give them advice or answer questions and be able to say whether it’s appropriate to go into the office or if it’s something that we can take care of at home.”
A number of remote medical sensors and other telemedicine devices have emerged in recent years.
Take a device developed by San Diego’s Sotera Wireless, for example.
The Visi Mobile System is able to measure and display all major vital signs through a sensor placed around the patient’s finger. It can wirelessly transmit the data to a desktop or tablet computer.
The Visi monitor is about the size of a iPhone. It's worn on the wrist.
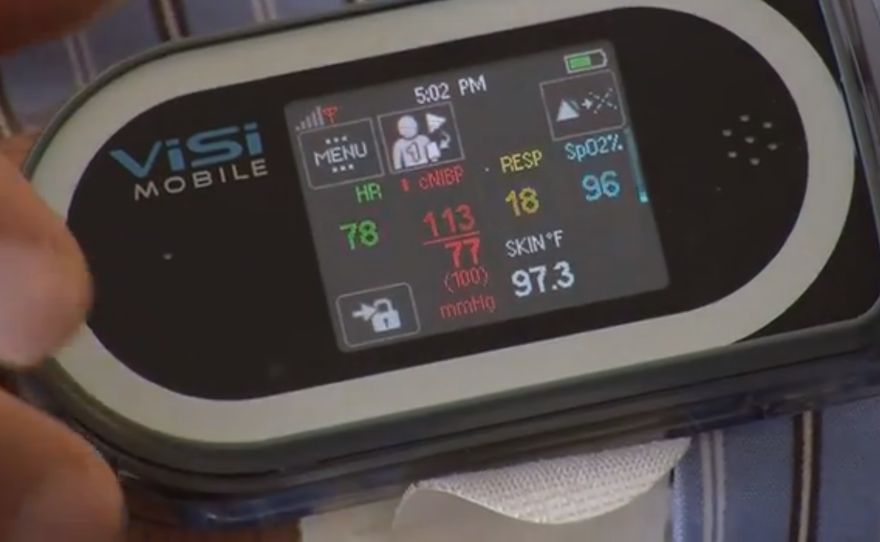
“You see on the top of the screen, I can see the actual cardiogram." said Dr. Eric Topol, director of the Scripps Translational Science Institute in La Jolla." Then, I want to look at the blood pressure waveform, so I have the blood pressure, and then here’s the waveform beat-to-beat of the heart. So basically what you have here is an intensive care unit on the wrist.”
The Translational Science Institute focuses on bringing the latest in wireless health technology to the patient.
Topol, a cardiologist said with devices like Visi, most patients could be monitored at home.
“That’s why the hospital of the future is really vulnerable," Topol explained. "Because why do you need a hospital, except for really sick people? Because most people will have their monitoring in their own home, or even on the go.”
But Topol is concerned that our medical system just isn’t fully prepared to embrace these innovations.
“These things are just now becoming available, just becoming a possibility," he said. "But typically in medicine, it takes many, many years before wide-scale adoption takes place. The average number is 15 to 17 years. We can’t wait that long. We need to innovate from the mess we’re in from a health care economic point of view.”
For the time being, only a relatively small number of health systems like Sharp Rees-Stealy are using remote medical devices to any degree.
As a result, there aren’t that many patients who are benefitting from them.
Steve White said he feels lucky to have his Cardiocom scale.
White hopes by keeping such close track of his condition and by taking care of himself, he’ll be able to beat the odds.
“I’ve done a lot in my time, so I feel that it’s all right, that I’m going to live with it the way it is, and do well. And baffle the congestive heart failure," White said.






