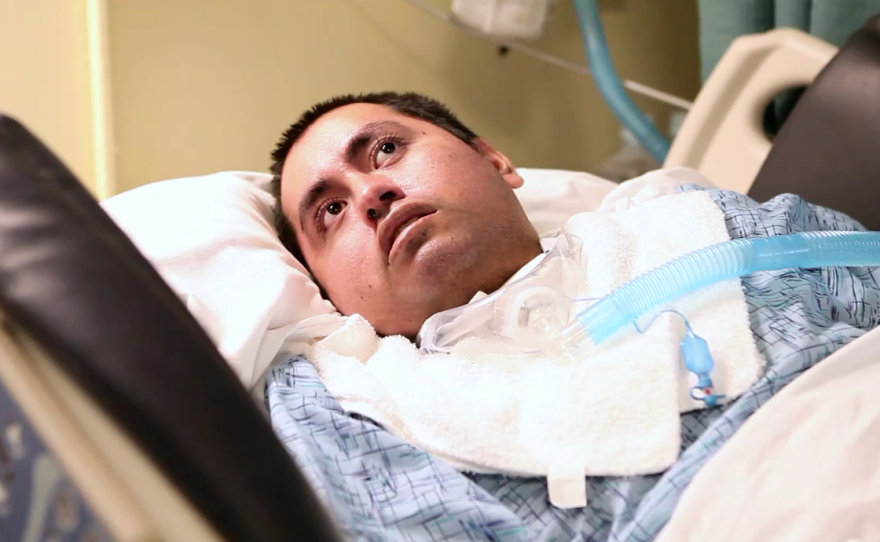
He smiles back at a reporter as she smiles and mouths the word “hello.” It’s an expression that belies both his official mental status — he’s believed to be non-responsive — and his circumstance. He has been lying in a nursing home bed for 15 years with a feeding tube in his stomach and a breathing tube in his throat.
Sixty-Six Garage, the random name he was given when he arrived at the UCSD Trauma Center in San Diego in 1999, is a John Doe who has been kept alive with machines since the vehicle he was traveling in crashed near the U.S.-Mexico border.
He can’t speak. Or walk. His atrophied limbs, his round face and his large brown eyes give him a child-like appearance, as though he’s been frozen in time. He couldn’t have been more than a teenager when he was thrown from the car, suffering a catastrophic brain injury.
Since inewsource made his story public late last year, at least a dozen families have come forward laying claim to Garage.
There was a desperate call to a reporter from a man on behalf of his wife — “She thinks it may be her son.” And a photocopy of a driver’s license with a handwritten note about a brother who went missing around the same time Garage was found, dropped off at the emergency room of a Sharp Hospital. Sharp HealthCare runs the Villa Coronado Skilled Nursing Facility, the place Garage lives.
And then there were two women who drove 100 miles from Riverside to Coronado to meet with Ed Kirkpatrick, the director of the nursing home, while their mother was on the phone in Nicaragua. So desperate to believe he might be her missing child she was attempting to arrange for a travel visa to the United States just to see him.
Others have called. Does he have a tattoo on his arm? He doesn’t. A birthmark on his back? None. A three-inch scar on his face? Only the large one across the left side of his head — from the accident that brought him to this place.
They have a “brief glimpse of hope,” Kirkpatrick said, that Garage may belong to them.
It’s a painful paradox to hope Garage - a man who needs 24-hour care, who cannot eat, who requires the mucus from his lungs be suctioned through a tube at least six times a day — is their son or brother. But like the mother on the phone from Nicaragua, these family members have been waiting more than a decade to know whether a son, or brother, is alive.
The Border Patrol reports that hundreds of migrants are found dead every year along the U.S.–Mexican border.
Many are never identified, according to the Colibrí Center for Human Rights in Arizona. The center attempts to identify remains and reunite them with their families. It has a database of 1,500 missing people last seen near the border.
A report last year by the International Organization for Migration estimated there were 6,029 deaths at the border between 1998 and 2013.
Enrique Morones, founder of Border Angels, a San Diego-based human rights group which provides aid and advocates for migrants, believes the actual number is much higher.
Morones said his group often finds bones in the desert. And he hears so many stories of missing people — the ones no one is accounting for. He often asks groups he speaks to in Mexico how many have lost a friend or loved one at the border.
“At first (years ago) it was a smattering of hands that would go up. Now there’s a smattering of hands that don’t go up,” he said.
Not knowing what happened to a missing person is the hardest part, Morones said.
“We get calls every week, every single week. ‘My brother crossed a few days ago. My mom crossed a few years ago, we don’t know what happened to her.’”
Keeping Garage alive
A nursing assistant removes the plastic cover protecting the tube in Garage’s throat. He inserts a hose, about the diameter of a pencil, into the opening of the tube. It’s attached to a small vacuum-like device.
It’s difficult to watch Garage’s face during the procedure. He turns red, his round cheeks inflate, and his eyes appear to be on the verge of tears. There’s an audible grating, sucking sound. Garage’s head jerks up and he lets out a muffled choking cough.
Kirkpatrick, the director of the nursing home, touches Garage’s arm to comfort him as the procedure is repeated.
“How would you like that done to you at least six times a day?” Kirkpatrick later asks.
The research isn’t clear about whether people with brain injuries like Garage’s feel pain.
He’s prone to seizures which can make him appear agitated. His arms and legs sometimes move spontaneously. On this afternoon, Garage’s arms are lifeless by his sides, his legs bent outward like an infant.
An inewsource investigation last September revealed there are more than 4,000 people living on special life support units across California. Garage is one of eight, according to the state, whose identities are unknown.
Their care, between $500 and $900 a day, is paid for by Medi-Cal, the state’s program for the poor and disabled. A section in the Medi-Cal policy manual allows Jane and John Does to qualify for care when they are comatose, amnesic, or in some other way incompetent.
There are also provisions in state policy that allow Medi-Cal to pay for long-term care for undocumented residents, a spokesman for the state told inewsource last year.
In California, the next of kin can decide to withdraw life-saving treatment, including food and water. Because Garage’s family has not been located and he can’t speak for himself, a team of doctors, healthcare administrators and a social worker make health care decisions on his behalf.
Why keep him alive? It’s a tough question to ask and even more difficult to answer.
Kirkpatrick, one of the people who help determine Garage’s medical treatment, isn’t sure what the right answer is legally or morally.
“I’m not sure, given the fact he is protected basically by the facility and the state, whether or not there would be other issues that would have to be addressed other than saying, ‘let’s say shut off the machines,’” Kirkpatrick said.
It’s an enormous challenge for a society to determine the right thing to do in these circumstances, said Charles Weijer, a philosopher and physician at Western University in Ontario, Canada, and a Canada Research Chair in Bioethics.
Weijer was in San Diego last week, to give a lecture about the ethics of neuroimaging in severely brain-injured people. He’s working with other researchers who have found a technique to determine whether people who are considered vegetative or minimally conscious, actually have some awareness and even the ability to process speech.
Their work found that one in five people who were considered non-responsive after a traumatic brain injury were actually consciously aware. When they were asked to imagine playing tennis or walk around their home, the results of their functional MRIs looked exactly the same as a healthy person.
The results are both hopeful and terrifying, posing more questions about quality of life, and specifically, whether people once thought of as unresponsive can feel pain.
With regard to Garage, Weijer would like to see an independent advocate, someone not associated with the nursing home, making decisions on his behalf.
“It seems problematic to me to have health care providers appointed as the decision makers on behalf of a patient,” Weijer said.
“There are real reasons to think there might be conflicts of interest.”
The nursing home may have to manage scarce resources.
For example, “needing to free up a bed so another patient can come in,” Weijer said.
Or at the other end, the nursing home is being paid to provide care — in other words — to keep Garage alive.
Ultimately, Weijer believes one day science could allow people like Garage to speak for himself, and tell doctors whether he is in pain and whether he wants to be kept alive.
The same neuroimaging techniques that can determine whether a non-responsive patient is aware, can also be used to communicate, he said.
Already, scientists in Canada have been able to successfully ask three people in a vegetative state yes and no questions by monitoring their brain activity while they were asked to perform a series of mental tasks. The researchers called it “brain-based communication.”
“I think further down the road ... is the possibility of actually gaining some insight into what’s it like to be in this state,” Weijer said.
“What sort of a life is this? I don’t think we’re ever really going to find out until we can ask the patient himself.”
Who is 66 Garage?
There is a sign above the bed that reads: Garage Sixty-Six. It begins, “I prefer to be called Garage or Sixty-Six.”
“I grew up in: Mexico,” it adds, which is the staff’s best guess.
The next two lines end in blanks: “My former occupation was…, and at home I live with…”
Morones, from the Border Angels, is encouraging the nursing home to continue telling Garage’s story, believing more publicity will help locate his family and ultimately determine his identity.
“The most important thing they (the nursing home) can do besides keeping him alive is getting the information out there,” Morones said.
He would also like to see the Mexican government get involved in the case and has offered to begin the conversation when he meets with that country’s undersecretary of tourism next month.
Kirkpatrick continues to answer the latest inquiries, most of which came after Garage’s story was posted on Facebook.
Kirkpatrick is using identifying information, things such as photos and birthmarks, to rule out the missing people who couldn’t possibly be Garage. If they make it past that first hurdle, a DNA test is next. So far, just one test has been done. A woman in Texas believed Garage might have been her missing brother and contacted the nursing home last year. The results were negative.
“We want to identify our Garage somehow, even if it has been 15 years,” Kirkpatrick said.