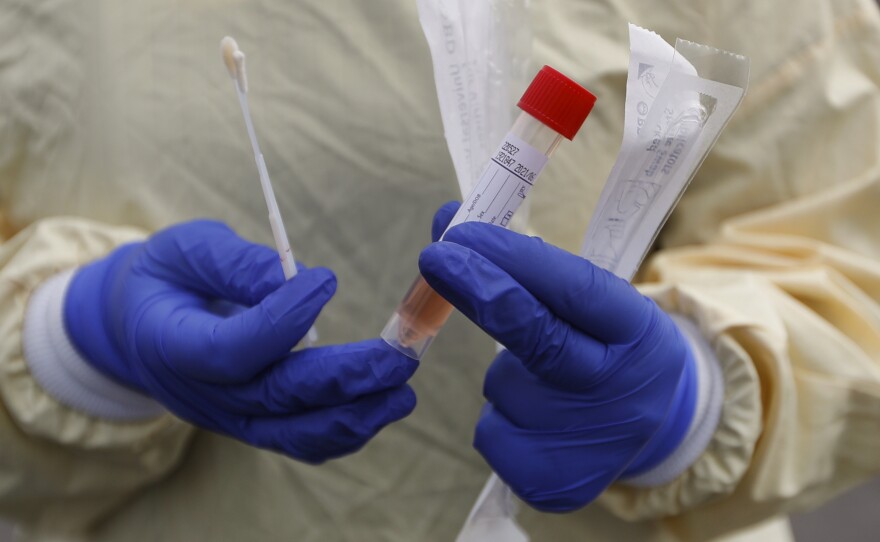
A second laboratory at UC San Diego Health launched specifically to handle COVID-19 tests has so far gone unused because the number of requested tests have been below what was expected.
Pathologist Dr. David Pride said UCSD worked to rapidly establish and expand testing capacity that would allow them to run up to 1,000 tests a day — plus another 600 if they opened the second lab — but in reality, its main lab is only processing about 300.
“The demand for our services hasn’t been what we thought it would be,” Pride said in a phone interview Friday.
San Diego County officials on Friday acknowledged the region’s facilities are not testing patients for coronavirus to the fullest extent possible, partially because of guidance that suggests limiting tests to only certain populations. The county’s public health officer announced a new task force to better utilize resources and possibly expand testing to more people.
In the meantime, at least two San Diego hospitals are loosening their own testing criteria and contracting with other facilities to take on their testing needs.
The Centers for Disease Control and Prevention recommend facilities prioritize severely ill patients or symptomatic individuals who are at a higher risk for the virus, including those with underlying medical conditions and health care workers. Testing should also be considered for those with mild symptoms in areas with a high rate of hospitalizations, the CDC said, but defers to doctors and health officials to make final decisions.
The guidance, which the county has said it follows, says patients without symptoms are not a priority.
Pride said the UCSD laboratory initially developed its own testing criteria focused on the most at-risk patients in order to conserve then-limited resources. As capacity increased, Pride said UCSD began to include those at lower risk.
“Over the course of weeks what we’ve done is very strategically add patient groups, and then add another and add another to the point at which we’re for the most part allowing for just about any physician to test their patients,” Pride said.
He said the laboratory also contracted with other entities to take on their testing needs, including for city of San Diego first responders, and is still negotiating with additional facilities.
Sharp HealthCare is taking similar steps to use its newly expanded capacity. The facility can process up to 950 daily tests but had been averaging around 124 a day until recently loosening its testing guidance. It's now planning to handle around 300 tests each day.
Sharp’s Dr. Omid Bakhtar said the gap is mostly because its inpatient needs didn’t accelerate as quickly as its testing abilities.
“There's only so many patients that you can see in a hospital at one time and so there's a certain need that you have in a hospital and I would say that that need isn't going to change too much,” pathologist Bakhtar told KPBS in a Friday phone interview.
Sharp expanded testing to cancer patients receiving treatment, those about to receive an operation and, as of Friday afternoon, women coming in for labor, spokesman John Cihomsky wrote in an email.
But Bakhtar said early on, restrictions were crucial because in-house abilities were previously limited to just under 100 tests a day.
“Physicians really had to think about, ‘do I really want to use one out of 96 tests on this patient when I have people on respirators in the hospital that need tests too?’” Bakhtar said.
The health care system is also using its additional capacity to handle tests for partner facilities and other institutions that may be relying on outside labs, which can take longer to receive results. Bakhtar said Sharp has been handling tests for Tri-City Medical Center for a couple of weeks.
Scripps Health reported seeing a lower demand for testing as well. Spokesman Keith Darcé said it is processing up to 250 each day even though it can handle up to 450.
“We are not seeing large numbers of symptomatic individuals coming to our hospitals that need testing, which is a sign that our providers are doing a very good job differentiating between those who could be positive and those with other issues,” Darcé wrote in an email Friday. “Our overall volume of patients seeking evaluation is also lower now.”
He noted the facility is not testing asymptomatic patients.
A spokesman for Palomar Health said Thursday the facility can test up to 60 patients a day, but is doing about half that because there wasn’t a greater demand for testing. However, a Kaiser Permanente spokeswoman said last week in an email “we are very near our limit,” but did not provide specific figures on daily tests and capacity.
San Diego County Public Health Officer Dr. Wilma Wooten on Friday announced a task force that would identify how to better use and increase the region’s testing abilities. She said stay-home orders and public messaging around who needs to be tested has prevented the region’s health care systems from becoming overwhelmed.
“The purpose of this task force is to convene county hospitals, relevant clinics and commercial laboratory systems that are responsible for testing throughout our county to look at how these individual systems can increase testing to the capacity that already exists as well as adding additional capacity,” Wooten said at the county’s daily new conference.
Wooten said that could include testing vulnerable populations, such as those living in long-term care facilities or low-income communities, but additional details would be shared at an upcoming board of supervisors meeting. Health care providers have begun testing all homeless individuals, regardless of symptoms, at the San Diego Convention Center.

However, Sharp’s Bakhtar warned against expanding to everyone because even though more than 2,000 people have tested positive for COVID-19 in San Diego County, the figure actually represents a low prevalence of the disease in the community and that could lead to inaccurate results.
“Any time you have low prevalence of disease, widespread testing of any type will have an immense number of false positives,” Bakhtar said. “That has nothing to do with the quality of your tests and everything to do with prevalence and epidemiology.”
He was especially wary of widely using antibody tests that may incorrectly report a person already had the illness and therefore cause that individual to no longer practice social distancing or other safety measures.
Pride said he wasn’t as concerned about false results, but said even with the current excess testing abilities, expanding the opportunity to more people too quickly could be problematic.
“If we open it up to everyone, then we probably would override our capacity really quickly,” he said.
At the same time, he said relaxing guidelines was important because hospitals may face financial troubles if they aren’t using the resources in which they significantly invested.
“At a time when most hospitals are hemorrhaging money, building excess testing capacity but not using it may make the problem worse,” Pride said in a follow-up email.
The next board of supervisors meeting is Tuesday morning. The Health and Human Services Agency is scheduled to present on its COVID-19 response.